Case contribution: Dr Radhiana Hassan
Clinical:
- A 48 years old man
- Underlying DM
- Presented with headache for the past 3 days
- Associated with lethargy
- No aggravating factor, no URTI symptoms, no fever, no vomiting, no body weakness
- Clinically vital signs are stable, GCS=14/15, pupils bilaterally reactive
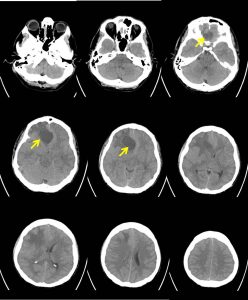
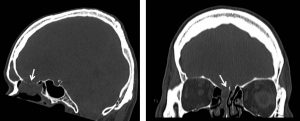
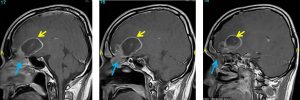
CT scan findings:
- There is a well-defined hypodense lesion at right frontal lobe measuring about 3.9cm(AP) x 3.5cm(W) x 3.4cm(CC) [average HU+25].
- Marked perilesional oedema is seen.
- Mass effect with midline shift towards the left about 12mm. Basal cisterns are effaced. Effacement of sulci with slightly poor grey white matter differentiation is noted.
- Extension of the lesion to the ethmoidal sinuses
- Bone erosion seen at cribifrom plate (white arrows).
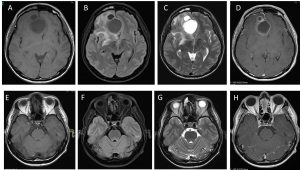
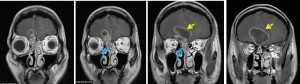
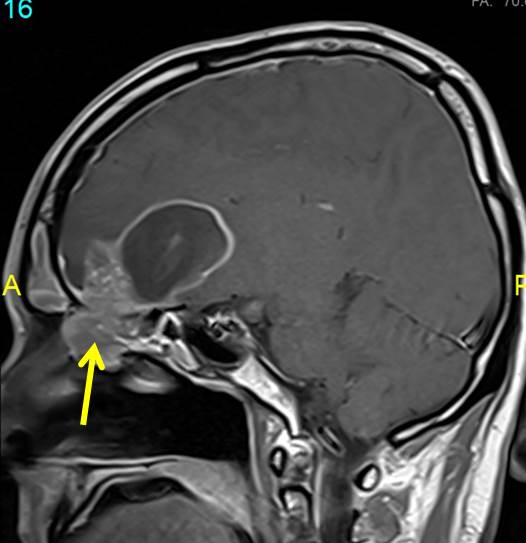
MRI findings:
- Large multicystic masses of varying sizes with rim enhancement are visualized in the right frontal lobe crossing midline to the left side
- It is causing shift of midline and subfalcine herniation to the opposite side.
- The largest cyst measures about 4.3 cm (AP) x 3.9 cm (TR) x 3.7 cm (SI) in size while the smaller cysts are located in close proximity anterior to it.
- Large peritumoural odema is observed.
- The mass abuts closely at the floor of the anterior cranial fossa with soft tissue extension to ethmoidal sinuses.
- The right frontal horn is obliterated but there is no hydrocephalus.
- No other lesion is seen elsewhere intracranially.
- No leptomeningeal enhancement.
- Enhancement also noted within the right frontal sinus.
- The visualized nasopharynx including the fossa of Rosenmuller and torus tubarius are normal.
Intraoperative findings:
- Bicoronal craniotomy and transphenoidal excision of tumour done by neurosurgical and ENT team
- Tumour with cystic and solid component seen
- Tumour is soft with moderate vascularity, straw coloured content
- Adhered to the frontal lobe
- Small defect at base of anterior fossa lateral to falx cerebri
- Friable tumour at olfactory cleft with abnormal ethmoidal and frontal mucosal sinuses
HPE findings:
- Macroscopy: specimen labelled as brain tumour consist of multiple pieces of whitish tissue
- Microscopy: section shows multiple fragmentn of lesional tissue with a fragment of normal-looking brain tissue. The lesional tissue is mainly crushed with areas of intact morphological features. The intact fragments show sheets of malignant cells displaying moderate nuclear pleomorphism with irregular vesicular nuclei, prominent nucleoli and scanty to moderate cytoplasm. There is marked lymphocytic and plasmacytic infiltrates seen within the surrounding stroma. The brain tissue is unremarkable with a focus of perivascular lymphocytic cuffing
- Immunohistochemistry: the malignant cells are diffusely positive for CKAE1/AE3 and are negative for LCA
- Interpretation: consistent with metastastic undifferentiated carcinoma.
Diagnosis: Sinonasal carcinoma with cerebral metastasis
Discussion:
- Sinonasal carcinomas are rare and account for 3% of all malignant tumours of head and neck
- The most common histological variant is squamos cell carcinoma. Other microscopic types include non-keratinizing scc, transitional cell ca, verrucous ca, basaloid scc, sarcomatoid ca, adenoca, small cell neuroendocrine ca and undifferentiated (anaplastic) carcinoma
- It occurs primarily in men aged 55-60 years
- Among paranasal sinuses, 76% cases are seen in ethmoidal sinus, 16% in sphenoid sinus, and 2% in frontal sinus
- Most common presentations are nasal obstruction, epistaxis and rhinorrhoea
- Intracranial invasion has the worst prognosis and was more frequent in mucinous subtype tumour.
- Sinonasal carcinoma is usually diagnosed late with extensive bone destruction at presentation.
- The prognosis of undifferentiated carcinoma is extremely poor. Median survival rate of less than 18 months and a 5-year survival rate of less than 20%.
- Local recurrence is common and metastatic disease occurs to cervical node with distant metastasis to bone, lungs, brain and liver
Recent Comments